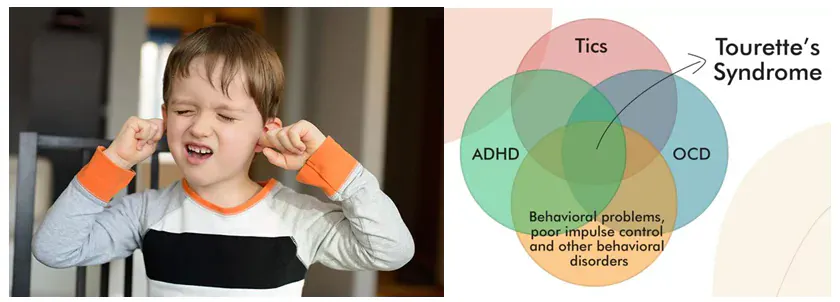
Tourette Syndrome (TS) & Tics
Quick Answer
If your child has sudden, repetitive movements or sounds they can’t control, it might be tics or Tourette Syndrome - but don’t panic! Most tics are temporary and many children outgrow them. Even children diagnosed with Tourette Syndrome can live completely normal, successful lives. The key is understanding, support, and working with your healthcare team. Remember: tics are NOT your child’s fault, and punishing them only makes things worse.
What Are Tics?
Tics are sudden, brief, repetitive movements or sounds that a person makes involuntarily (apne aap hone wali harkat). Think of it like a sneeze or hiccup - your child feels an urge building up and then releases it.
Types of Tics:
| Type | Examples |
|---|---|
| Motor Tics (Harkat wale) | Eye blinking, shoulder shrugging, head jerking, facial grimacing, jumping |
| Vocal Tics (Awaaz wale) | Throat clearing, sniffing, grunting, humming, repeating words |
| Simple Tics | Single, brief movements (eye blink, sniff) |
| Complex Tics | Multiple movements together or longer actions |
What Is Tourette Syndrome?
Tourette Syndrome (TS) is a neurological condition where a child has:
- Both motor AND vocal tics
- Tics occurring multiple times a day, nearly every day
- Tics lasting for more than one year
- Symptoms starting before age 18 Important: The media often shows people with Tourette’s shouting swear words (called “coprolalia”). This only affects about 10-15% of people with TS! Most children with Tourette’s never develop this symptom.
When Do Tics Usually Start?
Timeline:
- Peak onset: 5-7 years of age
- Worst phase: Around 10-12 years (puberty ke aas-paas)
- Improvement: Often decreases in late teens and adulthood
- Complete resolution: About 1/3 of children see tics disappear completely by adulthood Reassurance: Tics often look worse than they feel. Many children report the urge to tic is like an itch - uncomfortable until scratched but not painful.
What Causes Tourette Syndrome?
Known Factors:
- Genetics (Virasat): Often runs in families
- Brain chemistry: Involves dopamine and other neurotransmitters
- NOT caused by: Bad parenting, stress alone, vaccines, or anything you did wrong
Risk Factors:
- Boys are 3-4 times more likely to develop TS than girls
- Having a family member with tics or TS
- Premature birth or low birth weight (some studies suggest)
Recognizing Tics: What Parents Notice
Common Early Signs:
- Frequent eye blinking (baar baar aankh jhapakna)
- Throat clearing that doesn’t stop
- Facial movements or grimacing
- Shoulder shrugging
- Sniffing when not sick
- Sudden head movements
Tic Patterns:
- Tics change over time (one tic may replace another)
- They increase with stress, excitement, or tiredness
- They may decrease during focused activities (homework, games)
- They often reduce during sleep
- Children can sometimes suppress tics briefly (like holding back a sneeze)
When to Worry (Red Flags)
Consult your pediatrician if:
Tic-related concerns:
-
Tics are frequent and interfering with daily life
-
Tics cause physical pain or injury
-
Child is distressed, embarrassed, or avoiding activities
-
Tics have lasted more than a year
-
Multiple different tics (both motor and vocal) Other symptoms alongside tics:
-
Difficulty paying attention (ADHD symptoms)
-
Repetitive behaviors or thoughts (OCD symptoms)
-
Anxiety or depression
-
Learning difficulties
-
Sleep problems Sudden onset concerns:
-
Tics starting suddenly after infection (could be PANDAS)
-
Very severe tics appearing overnight
-
Tics with fever or behavior changes
Diagnosis: What to Expect
There is NO blood test or scan for Tourette Syndrome.
Diagnosis is based on:
- History: Doctor asks about tic types, duration, and pattern
- Observation: Watching for tics during examination
- Rule out other causes: May order tests to exclude other conditions
- Time: Must have tics for at least 1 year for TS diagnosis
Specialists who can help:
- Pediatric neurologist (Bachon ke brain specialist)
- Developmental pediatrician
- Child psychiatrist
- Clinical psychologist
Treatment Options
Good News: Many Children Need No Treatment!
If tics are mild and not bothering your child, you may just need to wait and watch.
When Treatment Is Needed:
1. Behavioral Therapy (Most Effective!):
- CBIT (Comprehensive Behavioral Intervention for Tics)
- Teaches child to recognize tic urge
- Trains competing response
- Very effective, no side effects
- Available in major Indian cities
- Habit Reversal Training
- Similar approach
- Works best for simple tics 2. Medications (Dawa):
| Type | Use | Examples |
|---|---|---|
| Alpha-agonists | First line, mild side effects | Clonidine (Arkamin) |
| Antipsychotics | For severe tics | Risperidone, Aripiprazole |
| Botox injections | For specific severe motor tics | Only in specialized centers |
Important: Medications don’t cure tics - they reduce them. Benefits must be weighed against side effects.
3. Managing Co-occurring Conditions:
- ADHD medication if attention issues present
- Therapy for anxiety/OCD
- Learning support if needed
Living with Tourette Syndrome: Practical Tips
At Home (Ghar Par):
DO:
-
Accept tics without drawing attention
-
Provide a “safe space” where child can tic freely
-
Maintain regular sleep schedule (neend ka routine)
-
Reduce stress when possible
-
Celebrate strengths and achievements
-
Talk openly about TS with child DON’T:
-
Tell child to “stop doing that”
-
Punish or shame for tics
-
Let siblings tease
-
Hover or watch constantly
-
Make tics the focus of family life
At School (School Mein):
Request accommodations:
-
Extra time for tests (tics can slow writing)
-
Breaks when tics increase
-
Seating away from distractions
-
Permission to leave class briefly if needed
-
Educate teachers about TS Talk to teachers about:
-
Not punishing for tics
-
Not asking child to suppress tics
-
Addressing bullying immediately
-
Focusing on child’s abilities, not tics
With Extended Family (Joint Family):
Common challenges and solutions:
- “Control kar, naatak mat kar” - Educate that tics are NOT drama
- “Kuch to kami hai” - Reassure that TS doesn’t mean low intelligence
- “Shaadi kaise hogi” - Many people with TS have successful relationships
- Share educational materials with grandparents, aunts, uncles
Associated Conditions
Children with Tourette Syndrome often have other conditions too:
| Condition | Percentage with TS | What It Means |
|---|---|---|
| ADHD | 50-60% | Attention and hyperactivity issues |
| OCD | 30-50% | Repetitive thoughts/behaviors |
| Anxiety | 30-40% | Excessive worry |
| Learning difficulties | 25-30% | May need extra academic support |
| Sleep problems | 25-50% | Difficulty falling/staying asleep |
Important: Sometimes these associated conditions cause more trouble than the tics themselves!
Resources in India
Where to Get Help:
- NIMHANS, Bangalore - Excellent pediatric neurology department
- AIIMS, Delhi - Comprehensive evaluation and treatment
- CMC Vellore - Specialized pediatric services
- Private pediatric neurologists - Available in major cities
Support Groups:
- Tourette Association of India - Online resources
- Parent support groups - Available on Facebook, WhatsApp
- School counselors - Can help with accommodation plans
Expert Insight: As our pediatricians remind parents: ‘Milestones have wide ranges. Focus on progress, not comparison.‘
FAQs
Q: Is Tourette Syndrome curable?
A: There is no cure, but many children improve significantly with age. About 1/3 of children see tics disappear completely by adulthood. For others, tics become milder and more manageable.
Q: Will my child shout bad words?
A: Probably not! The involuntary swearing (coprolalia) that media shows affects only 10-15% of people with Tourette’s. Most children never develop this symptom.
Q: Is this my fault? Did I do something wrong during pregnancy?
A: Absolutely not! Tourette Syndrome is a neurological condition with genetic factors. It’s not caused by anything you did or didn’t do. No bad parenting, no vaccine, no specific food causes TS.
Q: Can my child still succeed in life?
A: YES! Many successful people have Tourette Syndrome - doctors, lawyers, athletes, artists, businesspeople. With support and understanding, your child can achieve anything they set their mind to.
Q: Should I tell people about my child’s diagnosis?
A: This is a personal decision. However, educating teachers, close family, and friends often helps create a supportive environment. Let your child have input as they get older.
Q: My child’s tics get worse during exams. What can I do?
A: Stress increases tics - this is normal. Help with stress management, ensure good sleep before exams, request extra time if needed, and remind your child that tics during exams are okay.
Q: Are there any famous people with Tourette Syndrome?
A: Yes! International examples include soccer star Tim Howard, musician Billie Eilish, and many doctors, actors, and entrepreneurs. Many successful Indians have managed tics throughout their careers.
This article was reviewed by a pediatric neurologist. Last updated: January 2025
Concerned about your child’s tics or repetitive movements? Chat with Babynama’s pediatricians on WhatsApp for guidance on next steps.
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
Related Tools