All About Paediatric Pancreatitis In Children
Quick Answer
Pancreatitis in children is rare but can be serious. The good news: most cases of acute pancreatitis in children resolve completely within a week with proper care. If your child has severe upper stomach pain (pet ke upar bahut dard), especially with vomiting and fever, they need medical evaluation. While pancreatitis is uncommon, knowing the signs helps parents act quickly when needed.
What is Pancreatitis?
The pancreas is a large gland behind the stomach that:
- Produces digestive enzymes to break down food
- Makes insulin to control blood sugar Pancreatitis means inflammation of the pancreas. When inflamed, the digestive enzymes can start digesting the pancreas itself, causing pain and other symptoms.
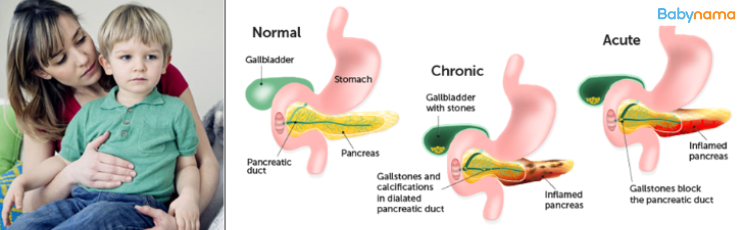
Types of Pancreatitis
| Type | Duration | Outlook |
|---|---|---|
| Acute | Few days to 2 weeks | Usually resolves completely |
| Recurrent Acute | Multiple episodes | Most children recover well |
| Chronic | Long-term | May need ongoing management |
Reassurance for parents: Most children who get pancreatitis experience only one episode and recover fully.
Causes of Pancreatitis in Children
Unlike adults (where alcohol is the main cause), children develop pancreatitis due to:
Common Causes:
-
Trauma/injury - Blow to abdomen (sports injury, accident)
-
Infections - Viral infections (mumps, other viruses)
-
Medications - Some medicines can trigger it (rare)
-
Gallstones - Less common in children than adults
-
Genetic factors - Family history of pancreatitis Conditions that increase risk:
-
Cystic fibrosis
-
Celiac disease
-
Metabolic disorders
-
Very high triglyceride levels Important: In many cases, the exact cause cannot be identified (idiopathic).
Symptoms to Watch For
Acute Pancreatitis Symptoms:
Main symptoms (pramukhya lakshan):
-
Severe upper abdominal pain - Usually sudden onset
-
Pain may radiate to the back
-
Pain worsens after eating
-
Child may bend forward for relief Other symptoms:
-
Nausea and vomiting (ulti)
-
Fever
-
Loss of appetite
-
Bloated or swollen belly
-
Irritability (especially in younger children)
-
Child looks unwell
Chronic Pancreatitis Symptoms:
- Recurring stomach pain
- Greasy, foul-smelling stools (steatorrhea)
- Weight loss or poor weight gain
- Diarrhea
- Poor blood sugar control (rare)
When to Seek Medical Care
Go to Hospital/Emergency if:
- Severe, persistent stomach pain
- Vomiting that won’t stop
- Child cannot keep fluids down
- High fever with stomach pain
- Child appears very unwell, pale, or weak
- Signs of dehydration
See Doctor if:
- Recurring stomach pain after meals
- Unexplained weight loss
- Greasy or unusual stools
- Pain that doesn’t improve with home care
Diagnosis
Tests your doctor may order:
- Blood tests
- Amylase and lipase levels (pancreatic enzymes)
- Elevated levels suggest pancreatitis
- Imaging
- Ultrasound - To see pancreas and check for gallstones
- CT scan - More detailed view if needed
- MRI - Sometimes used for detailed imaging
Treatment of Pancreatitis
Acute Pancreatitis Treatment:
Mild cases:
-
Pain management
-
IV fluids
-
Rest for the digestive system
-
Gradual return to eating Severe cases may need:
-
Hospitalization
-
IV fluids and nutrition
-
Pain medication
-
Treatment of underlying cause
-
Rarely, surgery (for complications) Good news: Most children with acute pancreatitis recover within a week!
Feeding During and After Pancreatitis
During acute episode:
-
Initially: Nothing by mouth (NPO) to rest pancreas
-
Gradually: Clear fluids, then soft foods
-
Doctor will guide when to start eating Recovery diet:
-
Start with easily digestible foods
-
Advance slowly based on tolerance
-
Low-fat diet may be recommended initially
Diet Guide for Children with Pancreatitis
Foods to Choose (Achche Khaana)
During Recovery:
- Clear soups and broths
- Boiled rice and khichdi
- Idli, soft dosa (minimal oil)
- Boiled vegetables
- Roti (without ghee)
- Steamed fish or chicken (if non-vegetarian)
- Dal (without tadka initially) General Healthy Diet:
| Food Group | Good Choices |
|---|---|
| Grains | Whole wheat roti, brown rice, oats |
| Proteins | Dal, lean chicken, fish, egg whites |
| Vegetables | All vegetables (steamed/boiled) |
| Fruits | All fresh fruits |
| Dairy | Low-fat dahi, buttermilk |
Foods to Limit or Avoid
Avoid during recovery:
- Fried foods (samosa, pakora, chips)
- Very oily/greasy foods
- Full-fat dairy products
- Red meat
- Processed foods
- Sugary drinks and sweets Note: Once recovered, most children can return to normal diet. Long-term restrictions are usually not needed unless doctor advises.
Special Considerations
For formula-fed infants with pancreatitis:
-
Doctor will guide on formula choice
-
May temporarily need specialized formula
-
Regular formula (NAN, Lactogen, Similac, Aptamil) is usually fine for most conditions
-
Never change formula without medical advice For toddlers and older children:
-
Focus on balanced, home-cooked meals
-
Limit junk food and fried items
-
Adequate hydration is important
-
Small, frequent meals may be easier to digest
Step-by-Step Recovery Guide
Step 1: Follow Hospital Instructions
- Complete any prescribed medications
- Follow dietary guidelines given at discharge
- Attend all follow-up appointments
Step 2: Gradual Return to Normal Diet
Week 1-2 after recovery:
-
Soft, bland foods
-
Low-fat options
-
Small, frequent meals (5-6 times daily)
-
Plenty of fluids Week 2-4:
-
Gradually add more variety
-
Increase portion sizes
-
Monitor for any discomfort After 1 month:
-
Most children can resume normal diet
-
Continue healthy eating habits
Step 3: Monitor for Recurrence
Watch for:
- Return of stomach pain
- Vomiting after meals
- Changes in stool Report any concerns to your doctor.
Tips for Parents
- Keep follow-up appointments - Even if child seems fine
- Maintain healthy diet - Good habits prevent problems
- Know warning signs - Severe pain, vomiting, fever
- Manage stress - Stress can worsen digestive issues
- Ensure adequate hydration - Water, buttermilk, coconut water
Common Mistakes to Avoid
- Rushing back to normal diet - Give digestive system time to heal
- Giving oily/fried foods too soon - Even if child asks for it
- Ignoring recurring symptoms - Report any pain episodes
- Self-medicating - Always consult doctor for pain relief
- Skipping follow-up appointments - Important for monitoring
Long-term Outlook
Reassuring facts for parents:
-
Most children with acute pancreatitis recover completely
-
Single episode usually doesn’t cause lasting damage
-
Many children never have another episode
-
With proper care, children can live normal, healthy lives Children with chronic or recurrent pancreatitis:
-
May need ongoing dietary management
-
Regular monitoring by gastroenterologist
-
May need pancreatic enzyme supplements
-
Small risk of diabetes development (rare)
Expert Insight: As Dr. Sumitra says, ‘Fed is best. Formula is a completely valid choice and provides excellent nutrition.‘
FAQs
Q: Can pancreatitis happen in babies?
A: Pancreatitis is rare in infants but can occur, especially in premature babies or those with specific medical conditions. In breastfed or formula-fed babies, digestive issues are usually due to other causes. If your infant has severe stomach distension, vomiting, and seems very unwell, seek immediate medical attention.
Q: My child had pancreatitis. Can they eat normally again?
A: Yes, most children can return to normal eating within a few weeks after recovery from acute pancreatitis. Start gradually with easily digestible foods and progress to regular meals. Long-term dietary restrictions are usually not needed unless advised by your doctor.
Q: Is pancreatitis related to eating too much ghee or oil?
A: In children, pancreatitis is usually not caused by dietary fat (unlike in some adult cases). However, during recovery, a low-fat diet helps the pancreas heal. Once recovered, normal amounts of healthy fats are fine.
Q: Can formula cause pancreatitis?
A: Standard infant formulas (NAN, Lactogen, Similac, Aptamil) do not cause pancreatitis. Pancreatitis in infants is very rare and usually related to other medical conditions or birth defects. If your baby has digestive issues, it’s much more likely to be something else like colic, reflux, or milk allergy.
Q: How long does recovery take?
A: Most children with acute pancreatitis feel better within a week. Complete recovery usually takes 2-4 weeks. Your doctor will guide you on when your child can return to normal activities and diet.
Q: Will my child need surgery?
A: Surgery for pancreatitis in children is rare. Most cases are managed with supportive care (fluids, pain management, rest). Surgery might be needed only if there are complications like abscess or if gallstones are causing the problem.
This article was reviewed by a pediatrician. Last updated: January 2025
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!