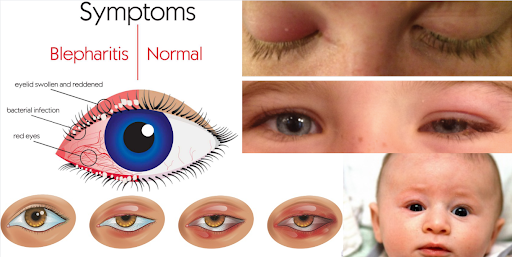
Pediatric Blepharitis: Causes, Symptoms, and Treatment
Quick Answer: Should I Be Worried?
Blepharitis (eyelid inflammation) is uncomfortable but usually manageable with proper care. If your bachcha has red, scaly eyelid edges with crusty lashes, especially in the morning, this is likely blepharitis. It’s a common condition that can come and go but is NOT dangerous when treated properly. The key is learning how to care for it at home - and we’ll show you exactly how!
What is Pediatric Blepharitis?
Blepharitis means inflammation of the eyelids. In children, it most commonly affects the edges of the eyelids where the eyelashes grow.
Think of it as: The small oil glands at the base of eyelashes getting clogged and irritated - similar to how dandruff affects the scalp.
Good news:
-
It’s not contagious (won’t spread to other children)
-
Usually doesn’t affect vision permanently
-
Can be managed with regular home care
-
Treatments are effective The challenge:
-
It tends to be chronic (comes and goes)
-
Needs consistent daily care to stay controlled
-
Can flare up during illness or allergy seasons
What Causes Blepharitis in Children?
Main Causes:
1. Bacterial Overgrowth
-
Normal skin bacteria multiply too much
-
Causes irritation and inflammation
-
Most common cause 2. Blocked Oil Glands (Meibomian Gland Dysfunction)
-
Tiny oil glands in eyelids get clogged
-
Oil becomes thick and doesn’t flow properly
-
Leads to dry, irritated eyes 3. Seborrheic Dermatitis Connection
-
Children with dandruff or cradle cap
-
The same condition can affect eyelids
-
Often runs in families 4. Skin Conditions
-
Eczema
-
Rosacea (in older children)
-
Psoriasis
Risk Factors:
- History of skin conditions in child or family
- Dry eyes
- Allergies
- Poor hygiene habits
- Rubbing eyes frequently
Symptoms by Age
Infants & Toddlers (0-3 years):
Since they can’t describe symptoms, watch for:
- Crusty eyelashes, especially on waking
- Red, swollen eyelid edges
- Rubbing eyes frequently (aankh ragadna)
- Fussiness during activities requiring vision
- Reluctance to open eyes in bright light
Preschoolers (3-5 years):
- May say eyes “hurt” or “itch”
- Visible crusty flakes on lashes
- Complaining about sandy or gritty feeling
- Light sensitivity
School-Age Children (5+ years):
Can describe symptoms like:
- Burning or stinging in eyes
- Feeling like something is in the eye
- Blurry vision (temporary)
- Tired, heavy eyelids
- Eyes tearing up
Home Treatment: Daily Care Routine
This routine should become as automatic as brushing teeth!
1. Warm Compress (Garam Sekai) - 2-3x Daily
What you need:
-
Clean washcloth or cotton pads
-
Warm (not hot) water How to do it:
-
Soak cloth in warm water and wring out
-
Have child close eyes
-
Place warm cloth over closed eyelids
-
Hold for 5-10 minutes
-
Re-warm as needed Why it works: Heat loosens crusts and melts blocked oil
Make it fun: Do during cartoon time, tell stories, or sing songs!
2. Lid Scrub (Palkon ki Safai) - 1-2x Daily
What you need:
-
Baby shampoo (Johnson’s, Himalaya) - just 2-3 drops
-
Cup of warm water
-
Clean cotton balls or soft cloth How to do it:
-
Mix baby shampoo with warm water
-
Dip cotton ball in mixture
-
Close child’s eye
-
Gently scrub along lash line in sideways motion
-
Use light pressure - don’t press hard
-
Use fresh cotton for second eye
-
Rinse with clean water
-
Pat dry Commercial alternatives: Lid scrub pads (Ocusoft, I-lid), available at pharmacies
3. Prevent Re-contamination
- Wash hands frequently
- Teach child not to rub eyes
- Change pillowcases 2-3 times per week
- Don’t share towels or washcloths
- Keep fingernails short and clean
When to See a Doctor
See an ophthalmologist (eye doctor) if:
-
Symptoms don’t improve after 2 weeks of home care
-
Eyes are very red and painful
-
Vision is affected
-
Significant swelling of whole eyelid
-
Thick pus discharge from eyes
-
Fever along with eye symptoms
-
Eyelashes falling out
-
Child seems very uncomfortable Your doctor may prescribe:
-
Antibiotic eye ointment (applied to lash line)
-
Antibiotic drops (for secondary infection)
-
Steroid drops (short-term for severe inflammation)
-
Oral antibiotics (for stubborn cases)
Long-Term Management
Daily Prevention (even when symptoms are gone):
-
Continue warm compresses once daily
-
Gentle lid cleaning as part of bedtime routine
-
Keep scalp clean if dandruff is present
-
Use humidifier in dry weather During Flare-ups:
-
Increase warm compress to 2-3 times daily
-
Be more rigorous with lid cleaning
-
Avoid eye strain (limit screen time)
-
Consider doctor visit if worsening
Expert Insight: Dr. Sumitra recommends: ‘Less is more with baby skin. Most rashes heal on their own with minimal intervention.‘
FAQs
Q: Is blepharitis the same as conjunctivitis (pink eye)?
A: No, they’re different. Blepharitis affects the eyelid edges, while conjunctivitis affects the white part of the eye. However, blepharitis can sometimes lead to conjunctivitis, and both can occur together.
Q: How long will my child have blepharitis?
A: Blepharitis is often a chronic condition that comes and goes. Some children outgrow it; others manage it into adulthood. The good news is that with proper care, symptoms can be well-controlled.
Q: Can I use regular soap to clean my child’s eyelids?
A: No! Regular soap can sting eyes and cause more irritation. Use diluted baby shampoo (no-tears formula) or commercial lid cleaning products designed for eyes.
Q: My child hates the warm compress. What can I do?
A: Try making it part of fun activities - during TV time, story time, or bath time. Use a favorite character washcloth. Start with shorter times and praise cooperation. Some children prefer warm cotton pads over a cloth.
Q: Will blepharitis affect my child’s vision?
A: Mild to moderate blepharitis usually doesn’t cause permanent vision problems. However, severe untreated cases can lead to complications. That’s why treatment and regular care are important.
Q: Can my child still go to school?
A: Yes! Blepharitis is not contagious. Your child can attend school normally. Just remind them not to share personal items and to avoid rubbing their eyes.
This article was reviewed by a pediatric ophthalmologist. Last updated: January 2025
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!