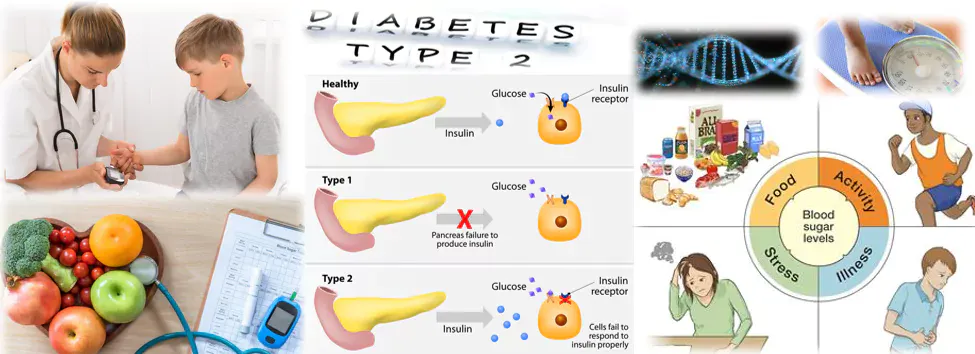
Type 2 diabetes in kids
Quick Answer
Type 2 diabetes in children is becoming more common, but it’s largely preventable and manageable with lifestyle changes! Once considered an “adult” disease, Type 2 diabetes now affects children too, primarily due to obesity and sedentary lifestyles. The good news: healthy eating and regular physical activity can prevent and even reverse early stages. If your child has risk factors, don’t panic - early action makes a huge difference.
What is Type 2 Diabetes?
In Simple Terms:
- Body doesn’t use insulin properly (insulin resistance)
- Blood sugar (glucose) builds up in blood
- Different from Type 1 (autoimmune)
- Develops gradually over time
- Often preventable Type 1 vs Type 2:
| Factor | Type 1 | Type 2 |
|---|---|---|
| Cause | Autoimmune | Lifestyle + genetics |
| Prevention | Not preventable | Largely preventable |
| Onset | Sudden | Gradual |
| Treatment | Always insulin | Diet, exercise, sometimes medication |
| Age | Any age, often children | Usually older, but increasing in kids |
Risk Factors
Who is at Risk:
-
Overweight or obese children (motapa)
-
Family history of Type 2 diabetes
-
Sedentary lifestyle (no exercise)
-
Poor diet (junk food, sugary drinks)
-
Certain ethnic backgrounds (South Asian included)
-
Prediabetes diagnosis
-
Signs of insulin resistance (dark skin patches)
-
Born to mother with gestational diabetes India-Specific Concerns:
-
High carbohydrate diet
-
Increasing junk food consumption
-
Reduced outdoor play
-
Screen time replacing activity
-
Genetic predisposition in South Asians
Warning Signs
Early Symptoms:
- Increased thirst (bahut pyaas)
- Frequent urination
- Increased hunger
- Unexplained weight loss
- Fatigue/tiredness
- Blurred vision
- Slow-healing cuts
- Dark patches on skin (neck, armpits)
- Frequent infections Note: Many children have no symptoms - testing is important if risk factors present!
Why This is Happening
The Modern Lifestyle Problem:
| Then | Now |
|---|---|
| Walk to school | Car/bus |
| Outdoor play | Screen time |
| Home-cooked food | Fast food |
| Water/lassi | Sugary drinks |
| Limited snacks | Constant snacking |
Contributing Factors:
- Processed food everywhere
- Large portion sizes
- Reduced physical activity
- More screen time
- Stress and sleep issues
- Cultural food practices
When to Worry (Red Flags)
Get your child tested if:
-
Overweight + family history of diabetes
-
Dark patches on neck or armpits
-
Excessive thirst and urination
-
Unexplained weight loss despite eating
-
Constant fatigue
-
Slow-healing wounds
-
Family history of diabetes Emergency Signs (Seek immediate care):
-
Fruity-smelling breath
-
Severe drowsiness
-
Rapid breathing
-
Vomiting
-
Confusion
What You Can Do
Healthy Eating
Do:
-
Whole grains (brown rice, ragi, oats, daliya)
-
Plenty of vegetables with each meal
-
Fruits in moderation (whole, not juice)
-
Lean proteins (dal, eggs, chicken, fish)
-
Healthy fats (nuts, ghee in moderation)
-
Water as main drink Avoid:
-
Sugary drinks (soda, packaged juice)
-
White bread, maida products
-
Excessive rice/potatoes
-
Packaged snacks (chips, biscuits)
-
Fried foods regularly
-
Hidden sugars in foods Indian Food Swaps:
| Instead of | Try |
|---|---|
| White rice | Brown rice, quinoa, millets |
| Maida roti | Whole wheat, multigrain |
| Sweet chai | Less sugar, unsweetened |
| Cold drinks | Nimbu pani, chaas, water |
| Packaged namkeen | Roasted makhana, nuts |
| Store-bought sweets | Homemade with less sugar |
Physical Activity
Daily Goals:
-
At least 60 minutes of activity daily
-
Mix of moderate and vigorous activity
-
Reduce sitting time
-
Limit screen to 1-2 hours Fun Activities:
-
Cycling
-
Swimming
-
Cricket, football, badminton
-
Dancing
-
Walking the dog
-
Playing in park
-
Traditional games (kho-kho, kabaddi)
Family Changes
Make it a Family Affair:
- Everyone eats healthy (not just the child)
- Active outings together
- Limit screen time for all
- Cook at home more often
- Set regular meal times
Treatment Options
Lifestyle Changes (First Line):
-
Healthy diet
-
Regular physical activity
-
Weight management
-
Regular monitoring Medication (If Needed):
-
Metformin (most common)
-
Other diabetes medications
-
Rarely, insulin Monitoring:
-
Regular blood sugar checks
-
HbA1c every 3 months
-
Regular doctor visits
-
Watch for complications
Prevention is Key
Start Early:
-
Breastfeed if possible
-
Delay sugary foods
-
Establish healthy eating habits young
-
Make activity part of daily life
-
Limit screen time from start
-
Model healthy behavior For At-Risk Children:
-
Get screened from age 10 (or puberty)
-
Annual screening if high risk
-
Early intervention for prediabetes
-
Healthy lifestyle is treatment
Frequently Asked Questions
Q: Mera bachcha mota hai - does that mean diabetes hoga?
A: Not necessarily, but excess weight (motapa) is a major risk factor. If your child is overweight, taking steps now to improve diet and increase activity can significantly reduce diabetes risk. Get screened if there’s family history too. Prevention is much easier than treatment!
Q: Can Type 2 diabetes be reversed in children?
A: Yes, especially if caught early! With significant lifestyle changes - healthy eating, regular exercise, and weight loss - many children can reverse Type 2 diabetes or prediabetes. The earlier you act, the better the chances. Work with your doctor to create an action plan.
Q: School mein unhealthy food milta hai - kya karun?
A: Pack healthy tiffin from home! Include protein (egg, paneer, dal), whole grains (roti, brown rice), vegetables, and a fruit. Talk to your child about making good choices. Request school to offer healthier options. Lead by example at home - children follow what they see.
Q: My child refuses to exercise - how do I motivate?
A: Make activity fun, not punishment! Let your child choose activities they enjoy. Join them - play together! Reduce screen time (creates boredom = motivation to play). Arrange playdates with active friends. Focus on making it enjoyable rather than “exercise for health.”
Q: Is Type 2 diabetes in children permanent?
A: Not always! With proper management, especially lifestyle changes, many children can achieve remission - meaning blood sugar returns to normal without medication. However, they remain at higher risk and must maintain healthy habits lifelong. Early intervention is key.
This article was reviewed by a pediatrician. Last updated: January 2025
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!