Insulin & Type 1 Diabetes in Children
Quick Answer
A diagnosis of Type 1 Diabetes is scary, but your child can live a full, active, healthy life! With proper insulin management, diet, and monitoring, children with T1D participate in sports, excel in school, and do everything other children do. This guide helps you understand insulin therapy and daily diabetes care for your bachcha.
Understanding Type 1 Diabetes (Madhumeha Samjhein)
What Is Type 1 Diabetes?
Key facts:
-
Body’s immune system destroys insulin-producing cells
-
NOT caused by eating too much sugar
-
NOT preventable - it just happens
-
Requires lifelong insulin (no cure yet)
-
Affects about 5% of all diabetics
-
Can start at any age (often childhood) Why insulin is essential:
-
Insulin = key that lets sugar enter cells for energy
-
Without insulin, sugar stays in blood (dangerous)
-
Your child’s pancreas can’t make insulin anymore
-
External insulin replaces what body can’t make
It’s NOT Your Fault!
Many parents feel guilty. Remember:
- You did NOT cause this
- It’s NOT from giving sweets
- It’s an autoimmune condition
- Good management = normal life
The Diabetes Care Plan
Four pillars of T1D management:
| Pillar | What It Means |
|---|---|
| Blood sugar monitoring | Check levels regularly |
| Insulin administration | Daily injections or pump |
| Healthy eating | Balanced diet, carb counting |
| Physical activity | Regular exercise |
Understanding Insulin Types
Types of Insulin
| Type | Onset | Peak | Duration | When Used |
|---|---|---|---|---|
| Rapid-acting | 15 min | 1 hour | 2-4 hours | Before meals |
| Short-acting | 30 min | 2-3 hours | 3-6 hours | Before meals |
| Intermediate | 2-4 hours | 4-12 hours | 12-18 hours | Twice daily |
| Long-acting | 2 hours | No peak | 24 hours | Once daily (baseline) |
Most children need combination:
- Long-acting (once daily) for baseline
- Rapid/short-acting (before meals) for food
How Insulin Is Given
Options:
- Insulin Injections (Syringes)
- Most common method
- Very thin needles (almost painless)
- 4+ injections daily typical
- Insulin Pens
- Pre-filled, convenient
- Easier dose measurement
- Good for school/travel
- Brands: NovoRapid, Lantus, Humalog
- Insulin Pump
- Continuous delivery through small tube
- No multiple daily injections
- More precise control
- More expensive option
Step-by-Step Injection Guide
Materials Needed
- Insulin vial or pen
- Syringe/pen needle
- Alcohol swabs
- Sharps container for disposal
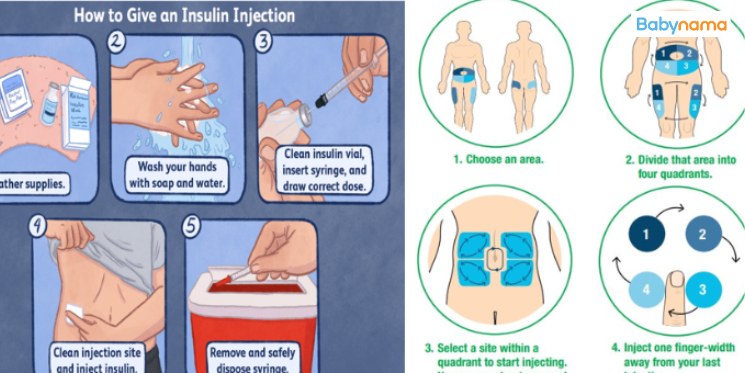
How to Give Injection
- Wash hands thoroughly
- Check insulin - not expired, correct type
- Clean injection site with alcohol swab
- Choose site (rotate locations):
- Abdomen (fastest absorption)
- Upper arms
- Thighs
- Buttocks
- Pinch skin gently
- Insert needle at 90 degrees (fully)
- Inject slowly
- Wait 5 seconds before removing
- Don’t rub the injection site
- Dispose of needle safely
Important Tips
Rotation is crucial:
- Don’t inject same spot repeatedly
- Use different areas of same site
- Leave 1 inch between injection spots
- Prevents lumps (lipohypertrophy)
Blood Sugar Monitoring
Target Ranges for Children
| Time | Target Range (mg/dL) |
|---|---|
| Before meals | 90-130 |
| 2 hours after meals | Less than 180 |
| Bedtime | 100-140 |
When to check:
- Before each meal
- Before bedtime
- Before/during/after exercise
- When feeling unwell
- If symptoms of high/low sugar
Recognizing Problems
Low Blood Sugar (Hypoglycemia) - Below 70:
Symptoms:
-
Shakiness, sweating
-
Hunger
-
Confusion
-
Irritability
-
Pale skin What to do:
-
Give 15g fast sugar (glucose tablets, juice, sugar)
-
Wait 15 minutes, recheck
-
If still low, repeat
-
ALWAYS keep glucose tablets handy! High Blood Sugar (Hyperglycemia) - Above 250:
Symptoms:
-
Excessive thirst
-
Frequent urination
-
Tiredness
-
Blurry vision What to do:
-
Check ketones (urine strips)
-
Give correction dose as per doctor’s plan
-
If ketones present, call doctor immediately!
Daily Life with T1D
School Management
- Inform teachers and staff about T1D
- Create diabetes management plan for school
- Pack supplies:
- Glucose meter
- Insulin/pen
- Fast-acting sugar
- Snacks
- Allow bathroom access (frequent urination when high)
- Exercise management during PE
Diet Tips (Khana Peena)
You don’t need “diabetic” food!
-
Focus on balanced, healthy meals
-
Learn carb counting
-
Pair carbs with protein/fat
-
Avoid sugary drinks (spikes blood sugar fast)
-
Time insulin with meals Indian diet tips:
-
Roti, rice, dal - count carbs
-
Include protein with each meal
-
Fiber helps (vegetables, whole grains)
-
Avoid sweets/mithai on regular basis
-
Fruits are OK - count the carbs
Exercise and Sports
Children with T1D CAN and SHOULD exercise!
- Check blood sugar before
- Have snack if below 100
- Carry fast-acting sugar
- Check after exercise
- May need to reduce insulin on active days
When to Seek Emergency Help
Call doctor or go to hospital if:
- Blood sugar very high (above 400) with ketones
- Vomiting and unable to keep food down
- Signs of DKA (diabetic ketoacidosis):
- Fruity breath smell
- Rapid breathing
- Confusion
- Abdominal pain
- Severe low blood sugar (unconscious, seizure)
- Unable to control blood sugars
- Child is sick with fever/infection
Emotional Support
This is hard for the whole family!
- It’s OK to feel overwhelmed initially
- Connect with other T1D families
- Don’t let diabetes define your child
- Gradually involve child in their care
- Celebrate management successes
- Seek counseling if needed
Frequently Asked Questions
Q: Insulin injection dard karti hai kya? Bachcha rota hai har baar.
A: Modern insulin needles are VERY thin - most children say it doesn’t hurt much. Tips: let insulin reach room temperature, use fresh needle each time, rotate sites, use numbing cream if needed, make it routine. Many children manage their own injections by age 8-10. Initial fear is normal and improves with time.
Q: Meetha khana bilkul band? Mithai kabhi nahi de sakte?
A: Your child can have occasional treats! The key is: count the carbs and give appropriate insulin. Birthday cake at a party? Yes, with proper insulin coverage. Daily mithai? Not recommended for anyone. Focus on balanced diet overall. Don’t make your child feel punished - manage, don’t ban.
Q: School mein insulin kaise manage karein?
A: Create a diabetes management plan with your doctor. Share with school: emergency contacts, injection schedule, hypoglycemia signs and treatment, foods allowed. Many schools have nurses who can help. Pack supplies in child’s bag. Older children can self-inject in school bathroom. Communication with teachers is key.
Q: Kya bachcha normal life jee sakta hai?
A: YES, absolutely! Children with T1D become doctors, athletes, engineers - everything! Many famous people have T1D. With good management, your child can: play sports, attend parties, travel, go to college - anything. T1D requires extra planning, not limitations. Focus on what they CAN do!
Q: Insulin pump better hai injections se?
A: Both work well. Pump advantages: fewer needle pokes, more precise dosing, better for active children. Disadvantages: cost (expensive in India), always attached, site changes needed. Many children do perfectly well with pen injections. Discuss with your endocrinologist what suits your child and family best.
This article was reviewed by a pediatrician. Last updated: January 2025
Newly diagnosed with T1D? Babynama’s pediatricians can help you understand daily management and answer your questions. Chat with us on WhatsApp!
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
