Insulin and Type 1 Diabetes in Children: A Comprehensive Guide
Quick Answer: Type 1 diabetes requires lifelong insulin because the body can’t produce its own. Children need multiple daily insulin injections or an insulin pump, along with careful blood sugar monitoring, balanced diet, and regular exercise. With proper management, children with Type 1 diabetes can live full, active lives. Work closely with your diabetes care team to create an individualized plan.
Understanding Type 1 Diabetes
Type 1 diabetes is an autoimmune condition where the pancreas stops producing insulin. Unlike Type 2 diabetes, it’s not caused by diet or lifestyle and cannot be prevented.
How It Differs from Type 2
| Type 1 Diabetes | Type 2 Diabetes |
|---|---|
| Autoimmune - body attacks insulin cells | Body doesn’t use insulin properly |
| Usually starts in childhood | Usually starts in adulthood |
| Always requires insulin | May be managed with diet/pills |
| Not related to weight | Often related to weight |
| Cannot be prevented | Can sometimes be prevented |
Understanding Insulin
What Insulin Does
- Moves sugar (glucose) from blood into cells
- Provides energy to the body
- Without it, sugar builds up in blood
- Without insulin, the body can’t use food for energy
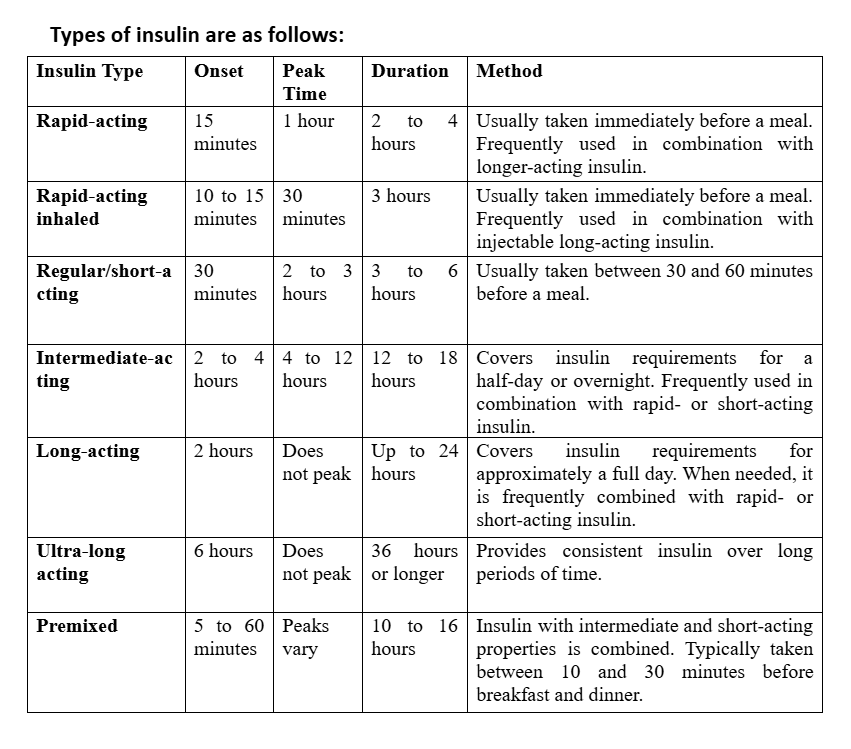
Types of Insulin
| Type | Onset | Peak | Duration | Used For |
|---|---|---|---|---|
| Rapid-acting | 15 min | 1-2 hrs | 3-4 hrs | Mealtime |
| Short-acting | 30 min | 2-3 hrs | 5-8 hrs | Mealtime |
| Intermediate | 2-4 hrs | 4-12 hrs | 12-18 hrs | Background |
| Long-acting | 2-4 hrs | No peak | 24+ hrs | Background |
Common Insulin Regimens
Multiple Daily Injections (MDI):
-
Long-acting once or twice daily
-
Rapid-acting at each meal
-
Most common approach Insulin Pump:
-
Continuous delivery of rapid-acting insulin
-
Programmable basal rates
-
Bolus doses at meals
Administering Insulin
Injection Sites
| Site | Notes |
|---|---|
| Abdomen | Fastest absorption |
| Upper arms | Good for children |
| Thighs | Common site |
| Buttocks | Slower absorption |
Injection Tips
- Rotate sites - Don’t use same spot repeatedly
- Room temperature - Cold insulin can sting
- Proper angle - Usually 90° for kids with adequate tissue
- Don’t rub - After injection, don’t massage area
- Stay consistent - Same site region at same time of day
For Young Children
- Use shorter needles (4-6mm)
- Distraction techniques help
- Let child choose injection site
- Praise cooperation
- Consider numbing cream if very anxious
Blood Sugar Monitoring
Target Ranges (General)
| Time | Target (mg/dL) |
|---|---|
| Before meals | 80-130 |
| 2 hours after meals | <180 |
| Bedtime | 90-150 |
Note: Your doctor will set specific targets for your child.
When to Check
- Before each meal
- Before bed
- Before and after exercise
- When feeling unwell
- When symptoms suggest high or low sugar
Tools for Monitoring
| Method | How It Works |
|---|---|
| Finger prick | Blood drop on test strip |
| CGM | Continuous sensor under skin |
Recognizing Highs and Lows
Low Blood Sugar (Hypoglycemia)
Signs:
-
Shakiness, trembling
-
Sweating
-
Pale skin
-
Hunger
-
Irritability, mood changes
-
Confusion
-
Dizziness Treatment (Rule of 15):
-
Give 15g fast-acting carbs (juice, glucose tabs)
-
Wait 15 minutes
-
Recheck blood sugar
-
Repeat if still low
High Blood Sugar (Hyperglycemia)
Signs:
-
Increased thirst
-
Frequent urination
-
Fatigue
-
Blurred vision
-
Headache Action:
-
Give correction insulin as prescribed
-
Increase water intake
-
Check for ketones if very high
-
Contact doctor if not improving
Diet and Nutrition
Key Principles
- Consistent carbohydrate counting - Match insulin to carbs
- Balanced meals - Include protein, fat, and fiber
- Regular timing - Helps stabilize blood sugar
- No forbidden foods - Can eat anything with proper insulin
Carbohydrate Counting
| Food | Carbs (approx) |
|---|---|
| 1 chapati | 15g |
| 1 cup rice | 45g |
| 1 apple | 15g |
| 1 cup milk | 12g |
| 1 slice bread | 15g |
Meal Planning Tips
- Include protein at each meal
- Choose whole grains over refined
- Include vegetables
- Limit sugary drinks
- Plan snacks if needed
Exercise and Activity
Benefits
- Improves insulin sensitivity
- Helps control blood sugar
- Maintains healthy weight
- Builds confidence
Precautions
| Before Exercise | During | After |
|---|---|---|
| Check blood sugar | Carry fast-acting carbs | Check blood sugar |
| May need snack if <100 | Watch for low symptoms | May need reduced insulin |
| Reduce insulin if needed | Stay hydrated | Monitor for delayed lows |
School and Social Life
School Plan
Work with school to create a diabetes management plan:
- Blood sugar checking times
- Insulin administration (if needed)
- Snack access
- Low blood sugar treatment
- Emergency contacts
- PE and activity guidelines
Telling Others
- Teach close friends about highs/lows
- Ensure teachers understand needs
- Child should carry medical ID
- Keep supplies accessible
Handling Sick Days
Important Rules
- Never skip insulin - Body needs more when sick
- Check blood sugar often - Every 2-4 hours
- Check ketones - If blood sugar >250
- Stay hydrated - Small sips frequently
- Contact doctor if vomiting, high ketones, or unable to eat
When to Seek Help
Contact Doctor If:
- Blood sugar consistently out of range
- Frequent lows or highs
- Illness lasting more than 24 hours
- Ketones present
- Weight changes
- Injection site problems
Emergency Signs:
- Unconsciousness
- Seizure
- Severe vomiting
- Signs of DKA (diabetic ketoacidosis)
- Unable to keep fluids down
Emotional Support
For Your Child
- It’s normal to feel frustrated, sad, or angry
- Connect with other kids with diabetes
- Focus on what they CAN do
- Celebrate management successes
- Allow age-appropriate independence
For Parents
- Join support groups
- Learn alongside your child
- Don’t blame yourself
- Take breaks when possible
- Seek help if overwhelmed
Frequently Asked Questions
Q: Can my child eat sugar with Type 1 diabetes?
A: Yes! Sugar isn’t forbidden. Children with Type 1 can eat any food as long as they take appropriate insulin to cover it. The key is learning how to count carbs and match insulin.
Q: Will my child always need insulin?
A: Currently, yes. Type 1 diabetes is a lifelong condition requiring insulin. Research continues on potential cures, but for now, insulin management is essential.
Q: Can my child participate in sports?
A: Absolutely! Many professional athletes have Type 1 diabetes. With proper planning - checking blood sugar, adjusting insulin, and carrying snacks - your child can be fully active.
Q: Is Type 1 diabetes genetic?
A: There’s a genetic component, but most children diagnosed don’t have a family history. It’s an autoimmune condition triggered by genetic and environmental factors.
Q: How do I handle birthday parties and treats?
A: Plan ahead! Know the food being served, count carbs, and give appropriate insulin. Your child can enjoy cake and treats just like other kids.
Key Takeaways
- Insulin is life-sustaining - Never skip doses
- Monitor regularly - Blood sugar checks guide insulin dosing
- Carb counting - Match insulin to food eaten
- Recognize highs and lows - Know the signs and treatments
- Normal life is possible - Sports, parties, and activities are fine
- Team approach - Work with your diabetes care team
This article was reviewed by pediatricians at Babynama. Last updated: January 2026
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!